Too impatient to get vaccinated?
Researchers from Konstanz and Switzerland examine willingness of Swiss hospital staff to get a COVID-19 vaccination – potential links to various behavioural factors and perceptions of social norms
What are the characteristics of the hospital staff who rejected getting a coronavirus vaccination when it first became available? This question is the focus of an interdisciplinary team of economists, behavioural scientists and health scientists from Konstanz (Germany) and Switzerland. Using survey data from two large Swiss hospitals, they look beyond the well-known socio-demographic factors, which tend to be related to the willingness to get vaccinated. The results appear in the current issue of PLOS ONE. Firstly, hospital staff who were hesitant to get the COVID-19 vaccination or rejected it altogether displayed a higher level of impatience compared to their vaccine-willing colleagues who were ready to get vaccinated right away. Secondly, they expected fewer people around them to get vaccinated. Since medical staff in particular serve the function of role models for the general public on health issues, this observation has implications for future health campaigns.
Hesitant despite serving as a role model
Since 15 March 2022, Germany has differed from some of its neighbouring countries (like Switzerland) in having a vaccination requirement for healthcare workers, a regulation that was recently confirmed by the Federal Constitutional Court. German legislators have one main goal with this partial vaccination requirement: protecting especially vulnerable groups, like people living in care homes or patients in the hospital. Independent of the requirement and its primary goal, there is another reason why the highest possible vaccination rate is desirable in the healthcare sector: Medical staff serve as role models for the general population.
"Healthcare workers often form a bridge between politics and patients. In medical matters, they act as a kind of informal opinion leader for their fellow citizens. Vaccination sceptics in healthcare can thus have a significant impact on the vaccination decisions made by the general public", says Ankush Asri, economist and behavioural scientist at the University of Konstanz, who is one of the lead authors of the study. This is one of the reasons for Ankush Asri and his colleagues to take a closer look at the differences between hospital staff who are willing to get vaccinated and their colleagues who are either hesitant to do so or who reject the vaccine altogether.
Surveys in two large hospitals
To get to the bottom of this question, the international team of researchers conducted a survey of staff in two large Swiss hospitals in January and February of 2021. A total of 965 persons took part in the survey. "At the time, the Swiss health authority had just approved the first COVID-19 vaccine – the routine vaccination of healthcare staff had not yet started", Viola Asri, a second lead author, explains. Participants in the study were asked whether they would get vaccinated, assuming the vaccine had been approved and was available for free. Possible responses were: "yes, as soon as it is available", "maybe later, when I have enough information" and "no, never".
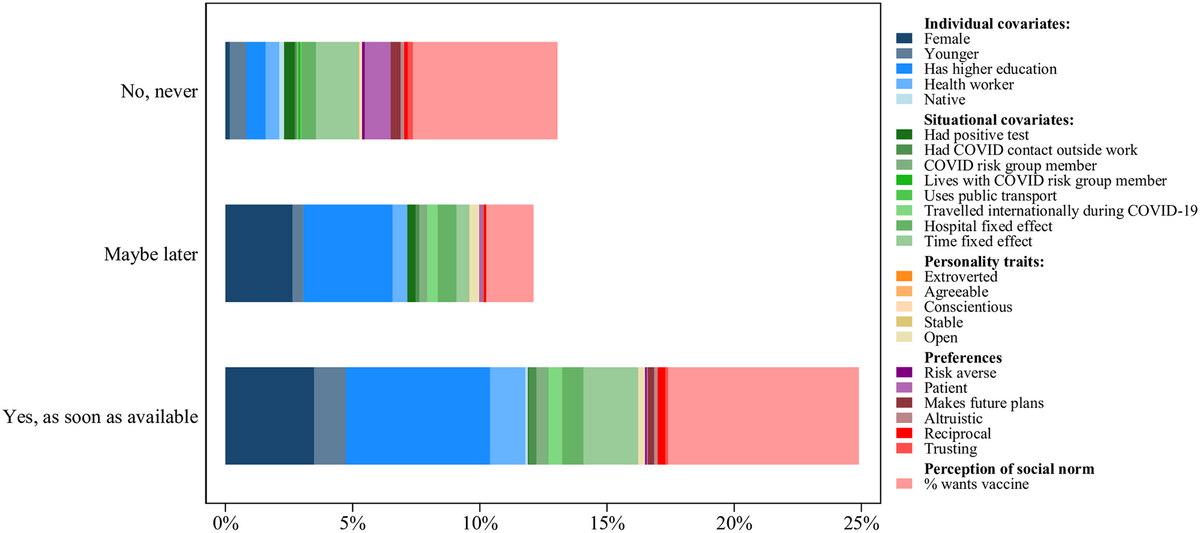
Along with this question, there were also questions involving socio-demographic factors so that correlations between the two could be examined. In addition, and in contrast to other comparable studies, the research probed other potential links to a range of standardized behavioural factors, including important personality traits, risk and time preferences as well as perceptions of social norms. "For example, the participants were asked to assess the level of vaccine willingness in their respective region. We used these answers to measure the individual perception of vaccine willingness as a social norm", Viola Asri adds.
Two prominent behavioural factors
The survey results confirmed known socio-demographic links. “For example, we observed that older age and higher level of education each increase the chances of a person being willing to get vaccinated immediately. The survey also revealed that the same is true for hospital staff who had been infected with the coronavirus before or who travelled internationally during the pandemic”, Baiba Renerte, a third lead author, explains.
The new insight was that behavioural preferences, such as patience – as measured by five test questions about whether one would prefer to get a small payment in cash right away or a larger payment later – or the perception of social norms, could play a role in vaccine willingness. The study revealed that “impatience” (in other words, unwillingness to do something now to benefit from it later) and the personal perception that vaccine willingness was low in the general public both increased the probability that hospital staff themselves either reject vaccination or are vaccine hesitant.
For the researchers, this means there are important implications for future health-related information and advisory campaigns. “We recommend that the messages used in the future for such campaigns should consider and make adjustments for “invisible” factors like perceived social norms and behavioural preferences. If you want to have the largest possible impact, it is not enough to only account for socio-demographic factors”, Baiba Renerte concludes.
Key facts:
- Original publication: Ankush Asri, Viola Asri, Baiba Renerte, Franziska Föllmi-Heusi, Joerg D. Leuppi, Juergen Muser, Reto Nüesch, Dominik Schuler, Urs Fischbacher (2022) Which hospital workers do (not) want the jab? Behavioral correlates of COVID-19 vaccine willingness among employees of Swiss hospitals. PLOS ONE;
DOI: https://doi.org/10.1371/journal.pone.0268775 - Surveys at two Swiss hospitals on COVID-19 vaccine willingness among staff members
- Findings of the survey: In addition to well-known socio-demographic factors, hospital staff members' patience and personal perception of the general public's vaccine willingness influence their own individual willingness to get vaccinated
- Recommendation of the researchers: To have the largest possible impact, health information and advisory campaigns should account for behavioural factors and perceived social norms along with socio-demographic factors