New approach prevents rejection of transplanted organs
Inhibition of a protein complex in cells of the immune system prevents rejection of transplanted organs – this has been shown in a study by immunologists from the University of Konstanz, the Biotechnology Institute Thurgau (BITg) and Chongqing Cancer University Hospital.
Organ transplants can save lives. Far too often, however, they fail because the patient's own body does not accept the foreign organ. What factors determine whether the body will accept a foreign organ? A Konstanz research team led by immunologists Michael Basler and Jun Li reveals: A protein complex in cells of the immune system, called the immunoproteasome, plays an important role, and future adjunctive therapies to organ transplantation could aim at inhibiting it.
Slow rejection of organs
If the donor and recipient do not completely match in organ transplantations, there is often a slow, gradual rejection of the foreign organ. "Transplant arteriosclerosis significantly contributes to chronic rejection and is a major reason for loss of function of the transplanted organ," Michael Basler explains.
The reason for rejection is the body's own immune defence: The body recognizes the new organ as foreign and initiates an immune defence against it. "In the first years after transplantation, you can prevent this effect well by suppressing the immune system," Basler explains. The immunologist from Konstanz has been researching a special protein complex in immune cells, the immunoproteasome, for years. Now he is studying its role in organ rejection.
The role of the immunoproteasome
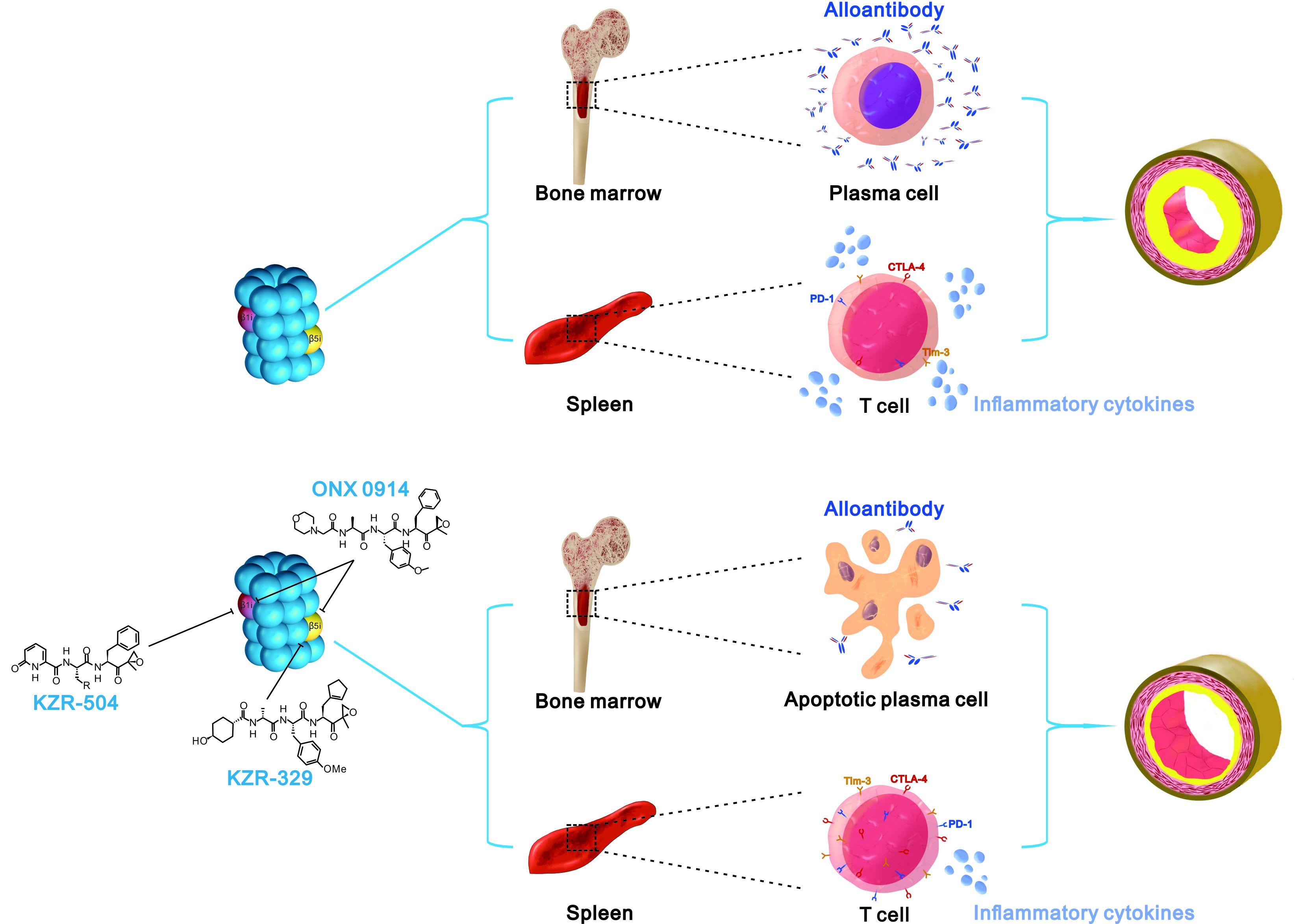
The immunoproteasome is a specific protein complex found in immune cells. Its task is to degrade proteins in cells. In plasma cells, antibodies are produced. Often they are misfolded – in a sense "defective" – and must be degraded by the immunoproteasome. If the immunoproteasome in these cells is inhibited, the defective antibodies can no longer be degraded and the plasma cells die. This way plasma cells that produce antibodies against the transplanted organ can be eliminated.
Drug treatment can very selectively inhibit and disable the immunoproteasome, which in turn weakens the immune system. What at first sounds like a disadvantage may very well make sense: namely, whenever the body's own immune system becomes a problem.
In years of research, the immunology research team based in Konstanz and Kreuzlingen showed that the inhibition of the immunoproteasome can be used to combat autoimmune diseases. The idea is to gently supress the immune system so that unwanted, harmful effects of the immune system no longer kick in. Hence, the immunoproteasome is a drug target to shut down the immune system in a controlled manner.
Prevent the rejection of the organ
The same effect can also be used to prevent the immune system from attacking and ultimately rejecting transplanted organs, as the research team led by Michael Basler and Jun Li showed in a recent study. By examining the transplantation of aortic vessels, they were able to demonstrate: Through inhibition of the immunoproteasome, the rejection of foreign organs is suppressed.
"In our publication, we demonstrated that atherosclerosis in the transplanted organ was prevented by immunoproteasome inhibition. In the absence of effective pharmacological drugs to prevent the chronic rejection of transplanted organs, immunoproteasome inhibition represents a new therapeutic approach that could improve the long-term prognosis of patients with transplanted organs," concludes Michael Basler. In his study the biological basis was explored. For the development of a medical therapy, further clinical studies will be required.
Key facts:
- Original publication: Jun Li, Shaobo Hu, Henry W B Johnson, Christopher J Kirk, Peng Xian, Yanping Song, Yuan Li, Nan Liu, Marcus Groettrup, Michael Basler, Co-inhibition of immunoproteasome subunits LMP2 and LMP7 enables prevention of transplant arteriosclerosis, Cardiovascular Research, 2022;, cvac181, https://doi.org/10.1093/cvr/cvac181
- The research results are based on a study with rats.
- The purpose of the study was to explore the biological basis. The therapeutic approach is not used yet. Further clinical studies are required for the development of a medical therapy.
- Research project of the University of Konstanz and the Biotechnology Institute Thurgau (BITg) as well as the Chongqing University Cancer Hospital (China).
- Funding provided by: German Research Foundation (DFG) and National Natural Science Foundation of China.


